Gynecologists Often Don’t Suggest *This* Non-Invasive Procedure That Spares Women a Hysterectomy — But They Should!
Yolanda Rhodes chose a painless, outpatient procedure proven to be 99% effective at eliminating fibroids

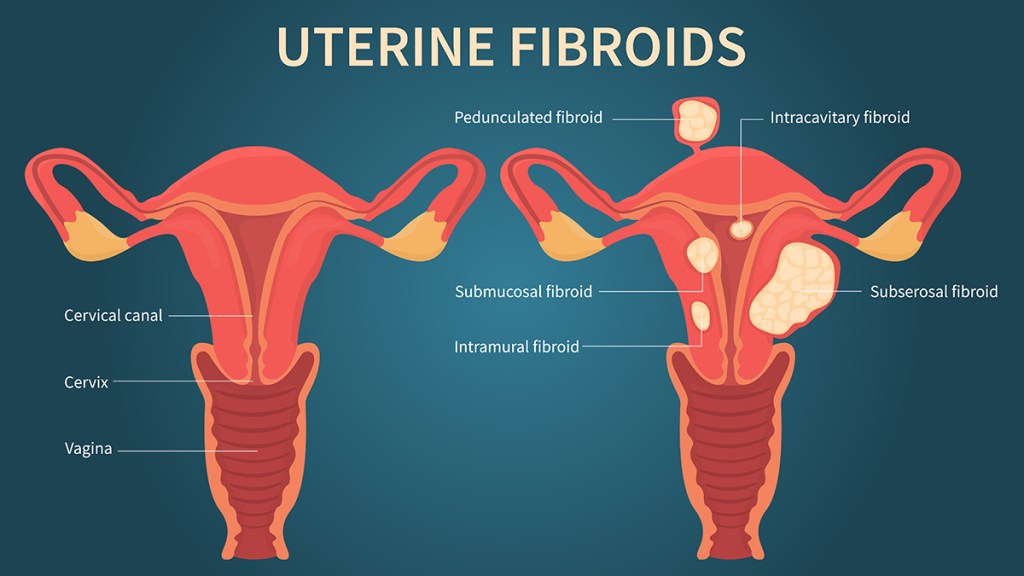
When fibroids — benign tumors that grow on uterine walls — lead to symptoms like heavy bleeding and pain, many doctors recommend hysterectomy. In fact, 30 percent of the 600,000 hysterectomies performed in the U.S. each year are done to resolve fibroids. But a hysterectomy is major surgery that comes with risks (from blood clots to pneumonia) and a four- to six-week recovery period. “The beauty of being a patient in 2023 is that there are other options that heal fibroids without surgery,” says gynecologic surgeon Linda Bradley, M.D., vice chair of the Cleveland Clinic’s Women’s Health Institute.
One of these is uterine fibroid embolization (UFE), a minimally invasive outpatient procedure where small, safe clotting particles are injected into the uterine arteries that supply blood to the fibroids. “When they’re starved of blood, the fibroids shrivel and shrink,” explains Dr. Bradley. It’s 90 percent effective, and recovery is typically a few days.
Gynecologists aren’t trained to do UFE (it’s done by an interventional radiologist), so some doctors don’t know to suggest it and will jump straight to hysterectomy. “If your doctor says you need a hysterectomy, unless it’s cancer, it’s never an emergency,” says Dr. Bradley, who encourages getting a second opinion. “Women need to know what UFE is and ask, ‘Why am I not a candidate?’”
Case in point: Yolanda Rhodes, 53, suffered from years of painful fibroids that resulted in heavy periods, bladder leaks, cramping. The registered nurse from Cypress, Texas feared her only option was a hysterectomy. But then her doctor suggested uterine fibroid embolization (UFE) and Yolanda had the simple outpatient procedure done. To her delight, it healed her pain and saved her from having a major surgery. Here, Yolanda shares her story.
Yolanda’s struggle with painful uterine fibroids
“What in the world?” Yolanda Rhodes said aloud as she walked into the bathroom. It felt like something inside her lower abdomen had dropped and fallen into her vagina. It didn’t hurt, but as a nurse, she knew something was very wrong. She grabbed a mirror and saw tissue protruding from her vagina, as icy terror washed over her.
While waiting for her OB-GYN to open, Yolanda did some research online and thought she had likely had a uterine prolapse, which happens when the muscles that support the uterus give out and it sags out of position. She suddenly remembered once having a patient with a rectal prolapse; she literally pushed it back in his body, which is called reducing the prolapse. Yolanda used the same process to gently push my uterus back in place with her fingers.
When Yolanda finally saw her doctor, she did an ultrasound. While Yolanda had previously been diagnosed with small, non-symptomatic uterine fibroids in the late 1990s, the scan showed these had grown significantly, weighing down her uterus and causing the prolapse.
“During the year before, I had started having very heavy, irregular and longer periods. I would get severe cramps and back pain. I was also leaking urine and losing my hair,” Yolanda tells FIRST for Women. “Because I was 49, we thought the symptoms were associated with the approach of menopause.” But she now discovered that her symptoms were the result of the fibroids growing. “I was terrified that I’d have to have a hysterectomy — like other women I know had.”
(Click through to our sister publication to discover natural ways to reduce your fibroid risk after menopause.)
She discovers hysterectomy isn’t the only solution
Yolanda was elated when her doctor said, “We have three options” and a hysterectomy was just one option. “I was a single mom with my youngest still in high school and I could only imagine the devastating toll taking a month off to recover from surgery would take on our lives,” Yolanda says. Her doctor also said that she could wear a birth control patch in the hopes of skipping all of her periods until menopause, though that might not alleviate all of her symptoms.
The third option was uterine fibroid embolization (UFE) — a minimally invasive procedure during which the doctor makes a very small incision in the wrist and inserts a catheter into the radial artery. This is guided by imaging to the uterus, where a safe clotting agent is delivered to the arteries supplying the fibroids with blood. Over a short time, the lack of blood makes the fibroids shrink.
“I spent two weeks deciding what to do,” Yolanda shares. “That whole time, my uterus would drop several times a day and I would have to push it back up. I finally called my doctor, crying, and asked for the name of a specialist who did UFE.”
Yolanda’s success with uterine fibroid embolization
Yolanda’s doctor referred her to Eric Hardee, M.D. who specializes in UFE with Texas Endovascular. “In June of 2019, I had the procedure, which thankfully was covered by insurance,” Yolanda says. “I went home a few hours later with just a Band-Aid on my wrist. I was a little nauseous and uncomfortable for a few days, but back to work in less than a week.”
Within a month, Yolanda had fewer prolapses each day. Within two months, all of her symptoms were gone. At six months, Yolanda’s OB-GYN confirmed my fibroids had shrunk back into the uterine wall, ending my prolapses. “I’ve since learned that African American women develop fibroids two to three times more frequently and at younger ages,” Yolanda reveals. “Many are only offered hysterectomy. I was fortunate my doctor recommended UFE and I was able to heal my fibroids without surgery. Today I still have no complications and the fear, pain, and embarrassment is gone. I have my life back!”
Click through for more ways to heal fibroids without surgery:
The 8 Best Ways To Prevent — And Shrink — Uterine Fibroids After Menopause
3 Easy Ways To Shrink Fibroids and Feel Better Fast
Uterine Fibroids: Everything You Need to Know About Treatment and Prevention
A version of this article originally appeared in our print magazine, First for Women.