Are You at Risk for Shingles? Docs Reveal Who *Can’t* Get the Virus + How to Calm a Flare-Up
Plus find out what you should do within the first 72 hours of a shingles rash to speed recovery
You may have heard the words shingles and chickenpox bandied about together, and for good reason — the two illnesses go hand in hand. Though you may think the chickenpox you had as a kid is one and done, it actually can show up again in your 50s and later. That begs the question, can you get shingles if you never had chickenpox? Here, doctors explain the link between the two conditions, what can spur a flare-up and the best home remedies to soothe a shingles outbreak.
What is shingles?
Shingles, also known as herpes zoster, is caused by the varicella-zoster virus (VZV), the same one that causes chickenpox as a kid. The Centers for Disease Control and Prevention estimates 1 in 3 people in the U.S. will develop shingles during their lifetime.
Symptoms of a flare-up include a painful, blistery and sometimes itchy rash. It typically occurs on the upper half of the body, such as the torso, chest and abdomen. “It appears as a stripe that curves around one side of the body and kind of looks like a shingle on a roof, hence the name shingles,” explains says William Schaffner, MD, professor of infectious diseases at the Vanderbilt University School of Medicine in Nashville, TN.
Besides showing up on the midsection of the body, shingles can also occur on the neck and face and in the ear or the eye. Other symptoms may include fever, chills, headache and stomach upset, the CDC reports.
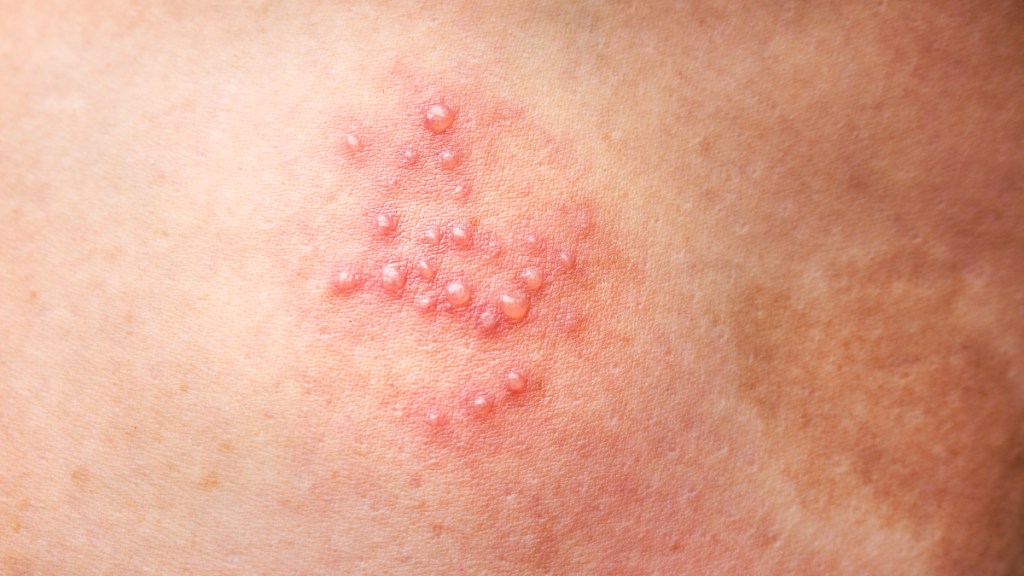
Shingles stages
While there are no formal shingles stages, the first sign of shingles is usually pain. People most often describe it as a stabbing, burning or tingling sensation, says Timothy Murphy, MD, an infectious disease doctor and a distinguished professor of medicine at the University at Buffalo. “About 24 hours after the onset of pain, someone with shingles will have fluid-filled blisters that appear on top of the rash,” says Dr. Murphy.
The blisters usually break in a day or two, then crust over, Dr. Murphy says. And the rash itself will most often clear up in about two to four weeks. However, the pain may stick around longer. This condition is called post-herpetic neuralgia (PHN). In most people, PHN goes away in 1 to 2 months.
Pain and the rash from shingles stems from the nerves in your body. That’s because the dormant chickenpox virus spends its retirement in your nervous system. “You recover from chickenpox, but the virus travels down to the nerve ends right under your skin,” says Dr. Schaffner. “When it’s reactivated, it actually irritates the nerves themselves and in doing so, stimulates pain fibers and the rash,” he explains.
Can you get shingles if you never had chickenpox?
Given that shingles stems from a previous chickenpox infection, you may be wondering if you can get shingles if you never had the chickenpox. Experts say the answer is no. “Nothing else causes shingles but the chickenpox virus, so the only people who can get shingles are those who have had chickenpox,” says Dr. Schaffner. Still, most adults are at risk of shingles. Why? The CDC reports that more than 99% of Americans born before 1980 have had chickenpox, even if they don’t remember it.
Unlike chickenpox, shingles is not contagious, so you can’t get it from another person. But there is a risk of someone with shingles passing on chickenpox to someone who never had it before. And chickenpox isn’t just for kids. Adults can get chickenpox if they never had an outbreak or haven’t been vaccinated for it. A chickenpox vaccine has been available in the U.S. since 1995. The CDC recommends two doses of the chickenpox vaccine for young children and adults who managed to skirt the condition.
Transmission of the virus to someone who never had chickenpox can happen via shingles blisters. “If you have fluid coming from the blisters and you come into contact with someone who never had chickenpox, that could transmit the chickenpox virus to another person,” says Susan Massick, MD, a board certified dermatologist and clinical associate professor of dermatology at The Ohio State University Wexner Medical Center. “You’ll be contagious until the blisters crust over and dry up.”
Top causes of a shingles flare-up
If you’ve had chickenpox as kid (as most of us have), you can experience a shingles outbreak in the future. Here are the most common triggers:
1. Age
As we get older, our immune systems weaken, says Dr. Murphy. “Certain chronic conditions that compromise the immune system can increase the likelihood of shingles, such as rheumatoid arthritis and type 2 diabetes,” Dr. Murphy says. These illnesses occur most often in middle aged or older adult, he adds. (At risk for diabetes? Click through for delicious food swaps for diabetes that curb your odds of developing the condition.)
2. Stress
A study in The British Journal of Dermatology found people who reported the highest levels of stress in their daily lives had an increased risk of shingles. Chronic stress may dampen cell-mediated immunity, which weakens the immune system and triggers the reactivation of the chickenpox virus.

3. Menopause
The North American Menopause Society reports that during menopause, women have higher rates of shingles than men. That’s most likely a result of changes in hormones such as lower levels of estrogen, contributing to a lower immune response to the virus. (Bothered by menopausal hot flashes, weight gain or mood swings? Click through to learn how probiotics for menopause symptoms can help.)
Can you get shingles more than once?
Yes, you can, though it’s not all that common, says Dr. Schaffner. In fact, the CDC found that most people who get shingles only have it once during their lifetime.
However, some people may be prone to a second or even third bout of shingles. Mayo Clinic researchers found recurrences of shingles were significantly more likely in people who had shingles pain of 30 days or longer the first time. Immunocompromised people, women and those 50 or older at the first shingles outbreak also have a greater chance of recurrence.
The best way to protect yourself from shingles is to get the Shingrix vaccine, which the CDC says is more than 90% effective at preventing the virus and its associated long-term nerve pain. The vaccine, which you can get at your doctor’s office or pharmacy, is for people 50 and older and is a two-dose process. The second dose is administered between 2 and 6 months after the first.
What you should do within 72 hours of a flare-up
If you do experience a shingles outbreak, the standard treatment is an antiviral medication prescribed by your doctor. “Antivirals can make shingles go away faster,” Dr. Murphy says. “But in order for these medications to be most effective, they should be started within 72 hours of the onset of symptoms.”
What is the best over the counter medicine for shingles?
To help manage shingles pain at home, you can take an over-the-counter pain reliever such as acetaminophen or ibuprofen, says Dr. Massick.
You can also try applying a cream containing capsaicin, a chili pepper extract that acts as a topical analgesic, to areas without broken skin or open blisters. It works by blocking chemical messengers’ ability to transmit pain signals to your brain. One to try: Zostrix Natural Pain Relief (Buy from Amazon, $15).
When it comes to itching, an oral antihistamine such as Benadryl can help. Calamine lotion, a go-to product used to relieve the itch from chickenpox as a kid, can also provide shingles relief if the rash is itchy, says Dr. Murphy. One to try: Caladryl Lotion (Buy from Amazon, $5.97).
3 shingles self-care tips
For added relief from a painful shingles flare up, try these simple remedies:
1. Wear loose-fitting clothing
“Shingles pain can be stimulated by all kinds of external sources such as a shirt or a blouse touching the area,” Dr. Schaffner says. “So it’s a good idea to wear clothing that’s not tight or going to rub against skin.”
Also smart: Choosing clothing with more breathable, natural fabrics such as cotton and linen that won’t catch on skin or contribute to irritation. You can also create a barrier between the rash and clothing by applying sterile gauze with medical tape on areas that are especially sensitive, says Dr. Murphy. (Click through to see our picks for the best loungewear that’s comfortable and has a relaxed fit.)
2. Take an oatmeal bath
Colloidal oatmeal, which is finely ground oats, has moisturizing and anti-inflammatory properties that calm skin and quell itchiness. You can make your own oatmeal bath by adding 1 cup of colloidal oats to lukewarm water (simply pulse whole, rolled oats in a blender or food processor until finely ground). Or try a pre-made soak such as Aveeno Colloidal Oatmeal Soothing Bath Treatment (Buy from Amazon, $7.57).

3. Apply a cold compress
Skip the ice pack in favor of a cool, moist compress, which tames inflammation, itching and pain. “A wet, cold washcloth can be better than using an ice pack for shingles because very cold temperatures may further inflame the blisters,” says Dr. Murphy.
Try applying a cool, damp compress several times a day for 5 to 10 minutes at a time. “People can use a bit of trial and error to figure out what feels good,” says Dr. Murphy. “If applying a cool compress provides good relief, than it’s fine to do it more frequently.”
For more ways to outsmart other viruses:
Eucalyptus Oil Is One of Nature’s Best Virus Killers, Says A Growing Body Of Research
How to Stop a Cold in Its Tracks: MDs Share Their Top Tips So You Can Feel Better Fast
These 3 Delicious Fruits Can Boost Your Immune System and Help Ward Off Viruses
This content is not a substitute for professional medical advice or diagnosis. Always consult your physician before pursuing any treatment plan.


















