Are Sinus Infections Contagious? Top MDs Answer This Surprisingly Tricky Question
Plus, the easy at-home remedy that often clears the infection without antibiotics
If you’ve ever experienced a sinus infection, you’re all too familiar with the congestion, discharge, bad breath postnasal drip, headaches, fatigue, fever and pain and pressure in the sinus cavities that can come along with it. You also likely have your go-to remedies. Still, you wonder: Are sinus infections contagious? In an ideal world, there would be a simple yes or no answer to this question. But the issue is not as straightforward as people would like it to be because the answer depends partly on what’s causing the sinus infection.
What is a sinus infection?
Many people and physicians have different ideas of what it means to have a sinus infection, based on categories of symptoms, according to a study in a 2022 issue of the International Forum of Allergy & Rhinology. But a sinus infection (also known as sinusitis) can be caused by a viral, bacterial or fungal infection — or even by allergies.
Research has shown a link between a deviated nasal septum — a common condition in which the wall of cartilage that separates the nasal passages is crooked — and a greater risk of sinusitis. In addition, having nasal polyps or having broken a bone in the mid-face can increase the risk of chronic sinusitis. Untreated, acute sinusitis can last up to four weeks, whereas chronic sinusitis lasts 12 weeks or longer.
Regardless of the underlying cause, when the sinus cavities are inflamed, mucus gets trapped and builds up, setting the stage for bacteria to grow and a sinus infection to occur. Sinus infections are actually quite common: More than 31 million people in the US have them each year, according to the American College of Allergy, Asthma & Immunology. (Click through to learn how a sinus infection can cause a crackling sound in your ear — plus how to get rid of the annoying noise.)
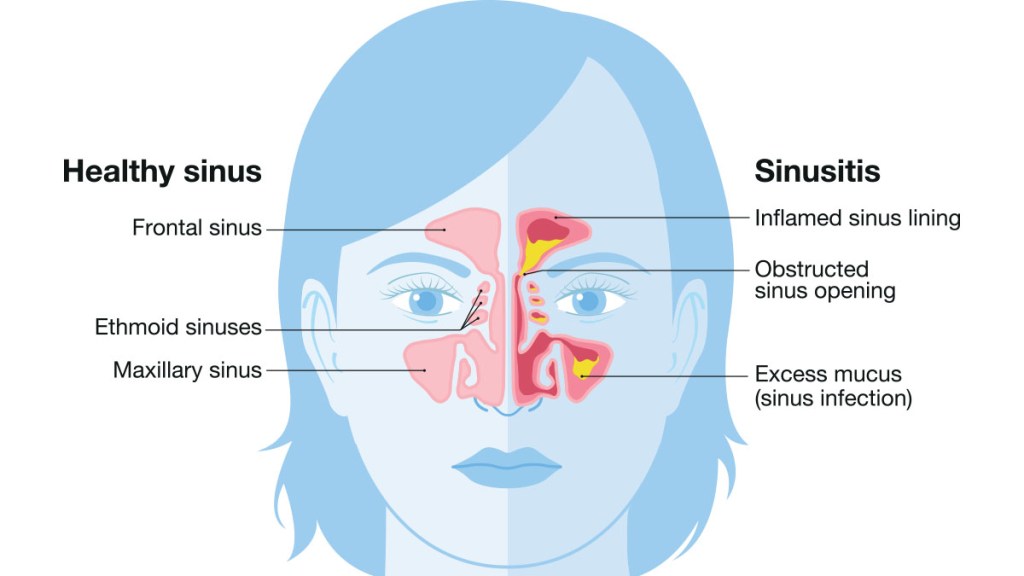
When is a sinus infection considered contagious?
“The question of contagion really comes down to what is the underlying cause,” says Ahmad Sedaghat, MD, PhD, a sinus specialist and an associate professor of otolaryngology at the University of Cincinnati College of Medicine. “Sinus infections are usually a complication of a viral upper respiratory infection.” In other words, sinus infections are usually secondary infections. They don’t happen on their own overnight.
Sinus infections that are a consequence of a viral infection
This is where things get complicated: If the underlying cause of a sinus infection is a virus (even one that causes the common cold), the virus can be transmitted to someone else, causing the person to catch the cold or other upper respiratory infection. But the sinus infection itself isn’t contagious or transmissible.
On the contagion issue, timing may come into play, too. “People often believe they have a sinus infection as soon as their sinuses get plugged, but a sinus infection tends to strike a week to 10 days after a cold,” says Kathryn Boling, MD, a family medicine specialist at Mercy Medical Centers in the Baltimore area. “If you get a cold and your sinuses are stuffed up, you’re contagious. It becomes a sinus infection when sinus drainage gets cut off and bacteria get trapped up there and start to grow there.”
Sinus infections that result from a bacterial infection
If a sinus infection isn’t preceded by an upper respiratory infection, it’s probably a bacterial infection, in which case it’s not contagious. “The bacteria that cause sinus infections typically live in people’s noses,” Dr. Sedaghat says. Also, if a sinus infection is a result of an upper respiratory infection and the symptoms persist beyond 10 days, it’s probably a bacterial infection and not contagious, he adds. Another possible sign of a bacterial sinus infection: If symptoms of an upper respiratory infection improve after day five but then worsen again, Dr. Sedaghat says.
Sinus infections that are caused by a fungal infection
Traditionally fungal sinus infections have been rare but they are becoming more common, Dr. Boling says. In fact, research has found that many fungal sinus infections have resulted from Covid-19 infections in recent years. The good news is that fungal sinus infections aren’t contagious. But they can be very serious, Dr. Sedaghat says. “These are surgical emergencies,” he says, “because they could be life-threatening” if the infection spreads into the brain. They’re more likely in people who have a weakened immune system. Fortunately, the combination of surgery and systemic antifungal drugs has improved the prognosis.
How do you treat a sinus infection?
You can often treat mild sinus infections at home — with over-the-counter pain relievers, nasal or oral decongestants, nasal steroid sprays and/or warm compresses on the face, Dr. Sedaghat says. It’s also important to stay well-hydrated to help thin out sinus secretions and get better faster, Dr. Boling adds.
The remedy to try before calling your doctor: a saline nasal spray. In a study in the journal Laryngoscope, people who used saline nasal sprays, which thin mucus and ease swelling, managed their sinusitis with 40% fewer antibiotics. That’s a good thing, since antibiotics can cause a host of side effects. You can find a wide variety of these sprays in your local drugstore.
If these steps don’t sufficiently ease your symptoms and a sinus infection persists longer than 10 days, your best bet is to contact your primary-care physician. A CT (computed tomography) scan or nasal endoscopy — in which a tech inserts a thin, flexible tube with a light and camera into the nose to provide a clear view of the sinuses and nasal passages — can confirm the diagnosis of chronic sinusitis.
In 2015, the American Academy of Otolaryngology-Head and Neck Surgery updated its clinical practice guidelines for treating sinusitis in adults: While emphasizing the importance of shared decision-making between patients and their physicians, the guidelines note that many cases of acute bacterial sinusitis can be managed with “watchful waiting” — watching to see if the infection clears up on its own — but antibiotics also may be appropriate.
Different doctors have different ideas about when it’s appropriate to start antibiotics for an acute bacterial sinus infection. (These drugs won’t help a viral sinus infection, though.) Keep in mind: “Most sinus infections require a longish treatment time — at least 14 days of antibiotics,” Dr. Boling says. These days, the gold standard is an antibiotic such as Augmentin (amoxicillin-clavulanate) but others may be used, depending on the patient’s situation and drug tolerance.
This content is not a substitute for professional medical advice or diagnosis. Always consult your physician before pursuing any treatment plan.
















