9 of the Best Devices for Improving Your Hearing for $300 or Less
It’s no secret that hearing aids are expensive. Top brands in the industry, such as Widex, Eargo, ZipHearing, Miracle-Ear, and even Costco’s line, Kirkland, are all priced in the $1,200 to $3,100 per unit range, making them a major investment by most standards. If you’re in need of a hearing aid but can’t cough up that kind of cash on a dime, it may make sense to consider a less costly hearing amplifier. Read on to find out which device is right for you.
Who needs hearing aids?
The Hearing Loss Association of America reports that around 20 percent of Americans — that’s 48 million people — have experienced some level of hearing loss in their lifetime. What’s more, according to the National Institute on Deafness and Other Communication Disorders (NIDCD), approximately 15 percent of Americans (37.5 million people) 18 and over report some trouble hearing, with age being the strongest predictor of hearing loss in adults aged 20 to 69. 60 to 69-year-olds, meanwhile, experience the greatest amount of hearing difficulties.
Needless to say, hearing aids are a necessary medical advancement for millions — particularly those in their golden years.
How do hearing aids work?
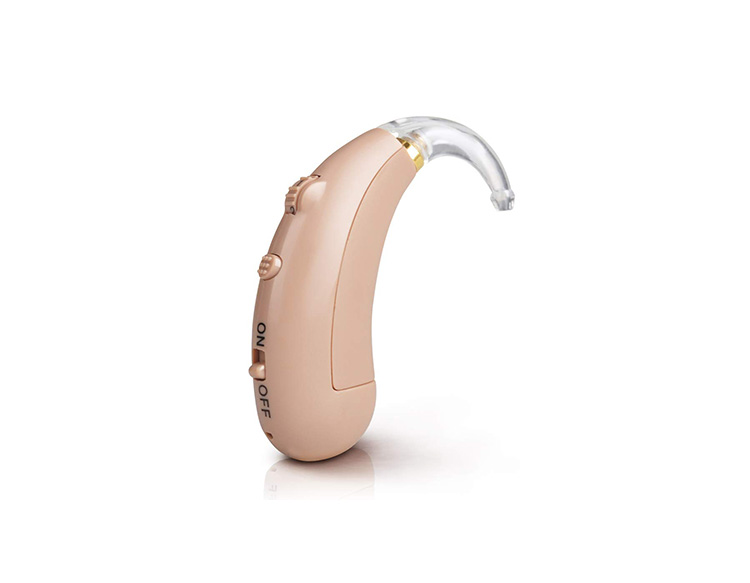
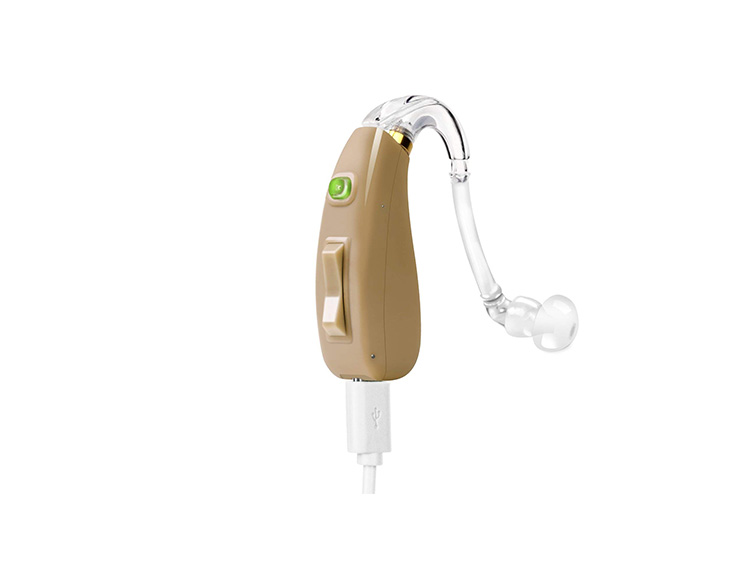
Hearing aids are small devices worn in or on the ear that make sound louder by magnifying vibrations which enter the ear. Each one has three main parts; a microphone, an amplifier, and a speaker. The microphone collects sound waves from the surrounding environment and converts them into electrical signals, which are then sent to the amplifier. The amplifier (a clever computer chip that is programmed with the specific needs of the wearer and converts sound into digital code based on the wearer’s level of hearing loss, level of surrounding sound, and listening needs) increases the volume of the sound waves and sends them directly to the ear via the speaker.
Can you get hearing aids with medical insurance?
The expensive price of hearing aids would be a non-issue for those with medical insurance if they were covered by traditional plans, but alas, more than half of insurance holders report that these essential hearing tools are subject to out-of-pocket funds. Similarly, Medicare coverage of hearing aids is dependent on state. According to one clinical review published in the Journal of the American Board of Family Medicine, “The Medicare Act of 1965 statutorily excluded coverage of hearing aids under the premise that they were ‘routinely needed and low in cost,’ suggesting that consumers would be responsible for their purchase.”
Luckily, there is an alternative for those seeking an efficient, more affordable — albeit temporary — solution to hearing woes: hearing amplifiers.
Hearing Aids vs. Hearing Amplifiers
Although these products are similar in design, there are a few major differences. Besides the cost of personal sound amplifying products (PSAPs), which begin as low as $40, PSAPs aren’t fully programmable and typically can’t be adjusted over the phone by professionals, like hearing aids can. Additionally, they’re not selective in which sounds they amplify, boosting all environmental noises uniformly.
Hearing aids, by contrast, are customized for the specific needs of the patient, from ear-shape to volume level and type of hearing loss. They can also serve as a suitable treatment for hearing loss.
Though PSAPs are intended for recreational use and aren’t meant to be a permanent solution to hearing loss, they can certainly come in handy in a bind. They also serve as temporary fixes for those who have misplaced or broken their hearing aids — a common occurrence — and are waiting for them to be repaired.
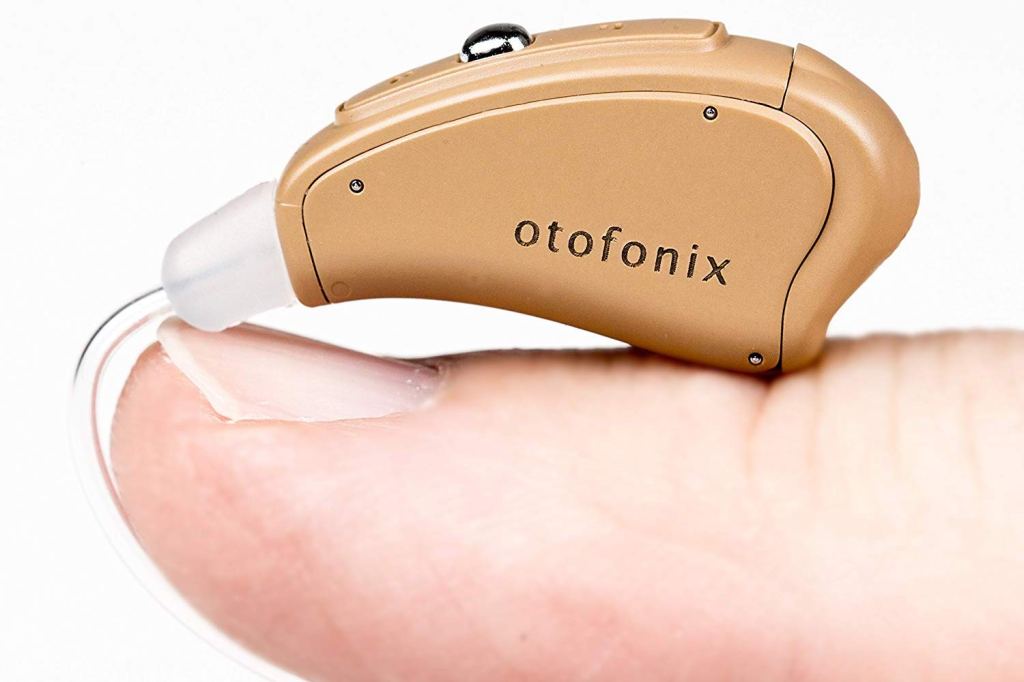
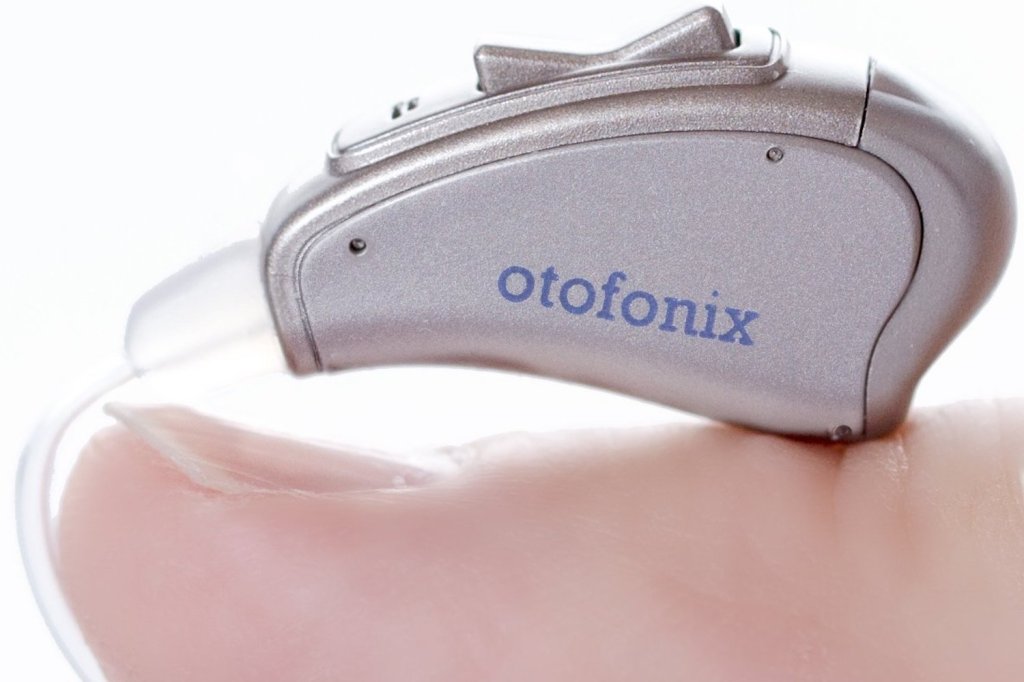
We’ve done deep research into the hearing amplifiers market to find nine great picks that range from $50 to $270, fitting both your budget and needs. Keep scrolling for FIRST’s picks for the best hearing aid amplifiers around.
We write about products we think our readers will like. If you buy them, we get a small share of the revenue from the supplier.